 
A few years ago, plan sponsors began adopting copay accumulator adjustment programs in their benefit designs. Puerto Rico have passed legislation banning state-regulated payer and PBM use of co-pay accumulator adjustment programs. Once these annual limits are reached, the plan pays for all subsequent prescriptions. Help us support Senator Swann (SB 1397) and Representative Rudder (HB 0619) in passing this bill. Normally, a manufacturer’s payments from a copay program count toward a patient’s deductible and annual out-of-pocket maximum. In recent years, payers and pharmacy benefit. It was most recently updated on Jto include new information. Note: This insight was originally posted on May 13, 2022. 1, 2024, about 13% of the commercial payer market will be operating under laws that ban accumulators. Tennessee currently has an active legislation to allow cost-sharing (co-pay) assistance to count towards a patient's deductible and out-of-pocket limit. If you’ve been using a drug manufacturer’s copay discount card to help with your out-of-pocket costs for a biologic or other specialty medication, you may soon be in for a surprise. 19 of people enrolled in the US commercial insurance market will belong to a health plan that must count copay assistance toward patient cost sharing by 2024. The bans are not just nibbling at the edges. IDF is pleased to announce that on ApArizona Governor Doug Ducey signed HB 2166 into law, making it the third state in the nation to ban co-pay accumulator programs. Some states’ laws ban co-pay accumulator programs outright, while others forbid their use unless the drug has a generic alternative. According to Avalere, as of January 2023, 16 states (Arizona, Arkansas, Connecticut, Delaware, Georgia, Illinois, Kentucky, Louisiana, Maine, New York, North Carolina, Oklahoma, Tennessee, Virginia, Washington and West Virginia) had banned accumulators in state-regulated health plans. As of summer 2023, 19 states have banned copay accumulators: Arizona, Arkansas, Colorado, Connecticut, Delaware, Georgia, Illinois, Kentucky, Louisiana, Maine. State regulators and legislatures have also gotten involved. District Court for the District of Columbia issued a decision vacating the Accumulator Adjustment Rule, regulations issued by the Centers for Medicare and Medicaid Services (CMS) in December 2020 as part of a Final Rule that addressed drug copay accumulator adjustment programs (the Rule). In August 2022, three patient groups - the HIV and Hepatitis Policy Institute, the Diabetes Patient Advocacy Coalition and the Diabetes Leadership Council - filed a lawsuit challenging a Trump administration decision that allowed pharmacy benefit managers to continue to use accumulator and maximizers. 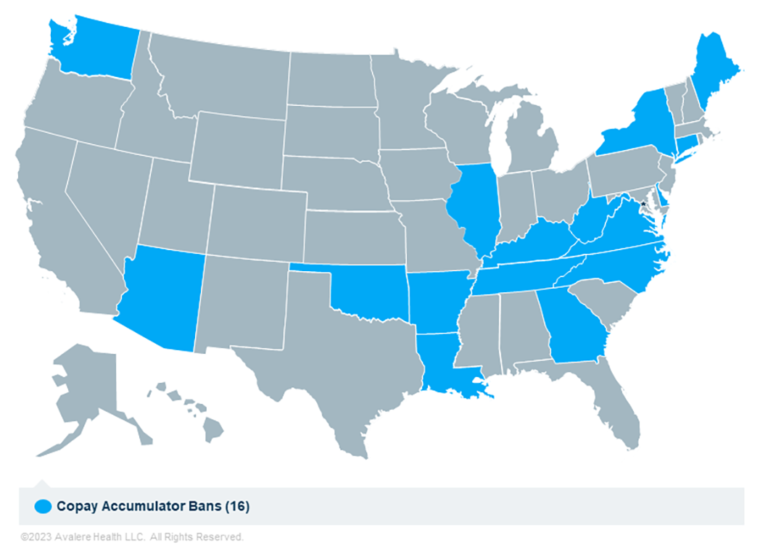
Many patient groups and professional organizers are opposed to accumulator programs. To address these challenges, Americans support patient-centered policy solutions that lower out-of-pocket costs, improve access and increase accountability.According to Avalere Health, a healthcare consulting firm in Washington, D.C., more than 80% of the people covered by commercial insurance belong to plans that have implemented a copay accumulator and more than 70% are in plans with copay maximizers, a version of the accumulators designed to even out patient out-of-pocket costs. UPDATED JUNE 15, 2023: The Copay Accumulator bill (SB-195) to protect co-pay assistance for patients passed the Colorado State Legislature and has now been signed by Governor Polis. 29% of insured Americans taking prescription medicines report being subject to utilization management practices, such as prior authorization or formulary exclusion, which can restrict or delay patients’ access to medicines 19% of insured Americans say their health care out-of-pocket costs are more than they could afford if they had a major unexpected medical event or were newly diagnosed with a chronic illness Too many Americans face repercussions of insurer and PBM practices that drive up health care costs, put up barriers between patients and their medicines and jeopardize access to new and innovative treatments. 
Insured Americans overwhelmingly say they believe that health insurance should provide affordable access to health care (93%), yet only a third (34%) say they believe it currently delivers, according to new data. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
